Description
Breast Reduction (reduction mammaplasty) is a surgical procedure performed to reduce breast size for a number of reasons:
- To reduce back, neck, and shoulder pain due to heavy breasts.
- To reduce skin irritation and rashes beneath heavy breasts.
- To balance breast size when the breasts are of different sizes.
Many women with enlarged breasts will experience neck, upper back, and shoulder pain. Other common complaints include deep shoulder marks from bra straps, poor posture, chronic irritation beneath the breasts, difficulty finding bras and clothing that fit properly, and inability to participate in sports activities.
Breast reduction is successful in reducing or eliminating these symptoms in 95% of women. The procedure is accomplished by removing variable amounts of breast tissue and skin, tightening and lifting the breast, and decreasing its size. The areola (pigmented skin surrounding the nipple) is also reduced in size and elevated. Dr. Friedman generally performs liposuction to remove excessive fat along the outer part of the torso adjacent to the breast.
Female Breast Reduction Before and After Photos
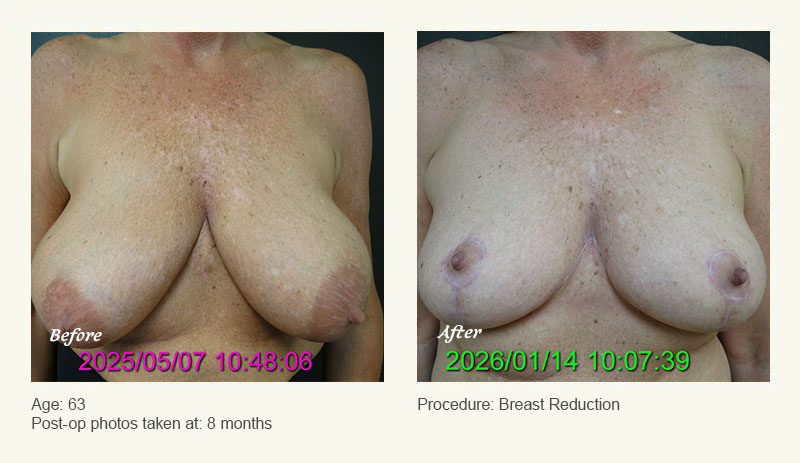
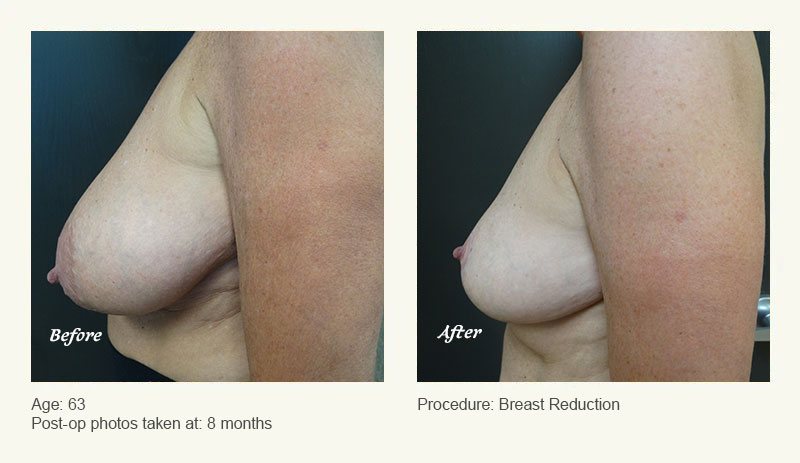
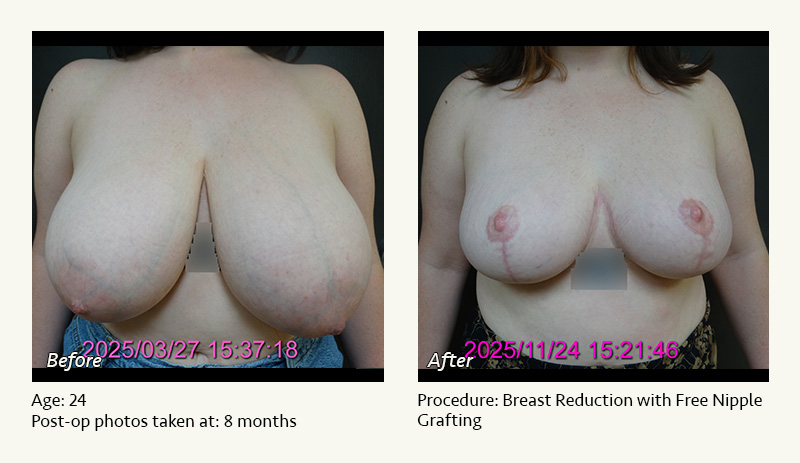
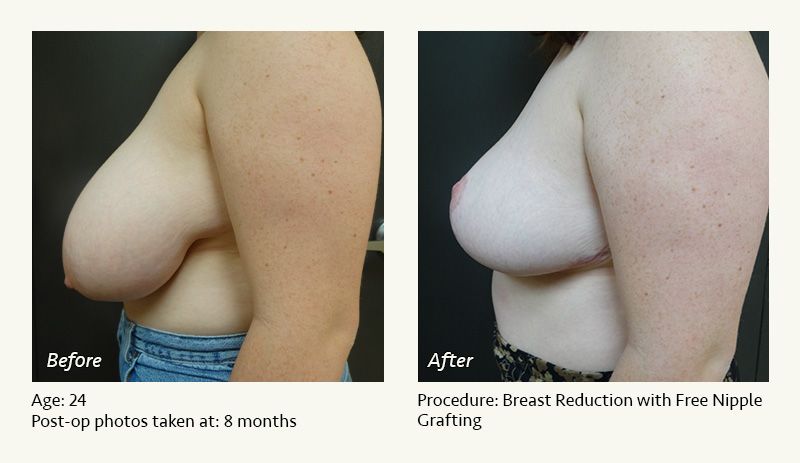
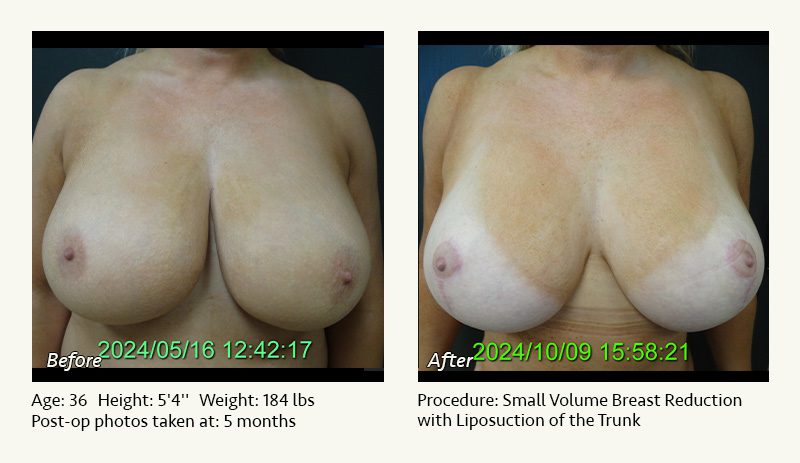
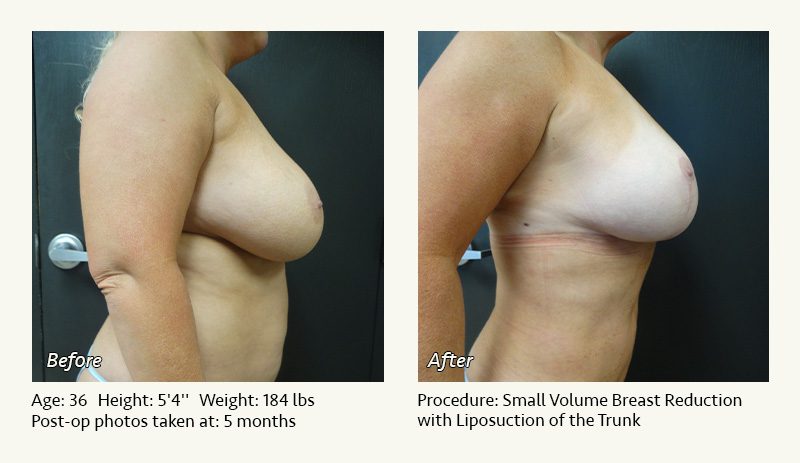
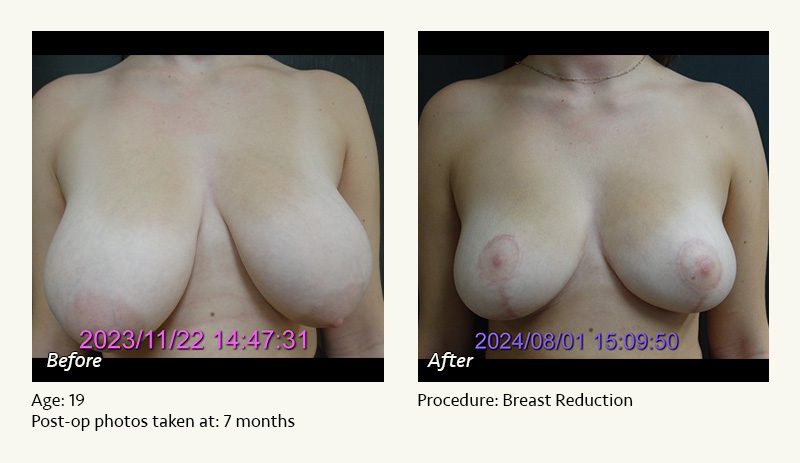
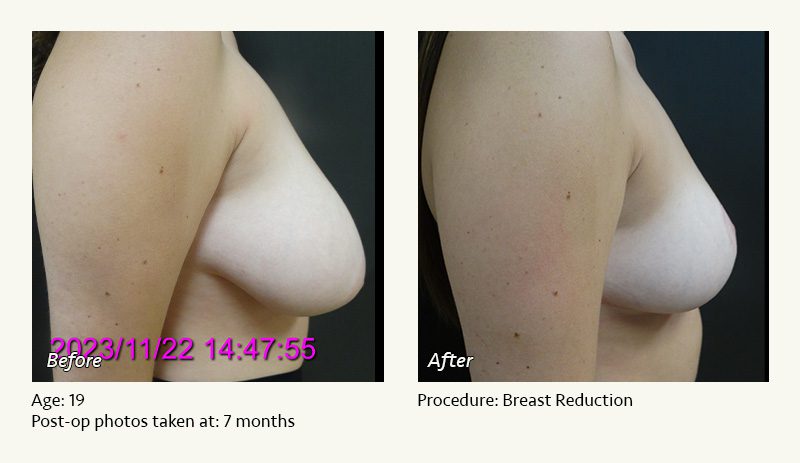
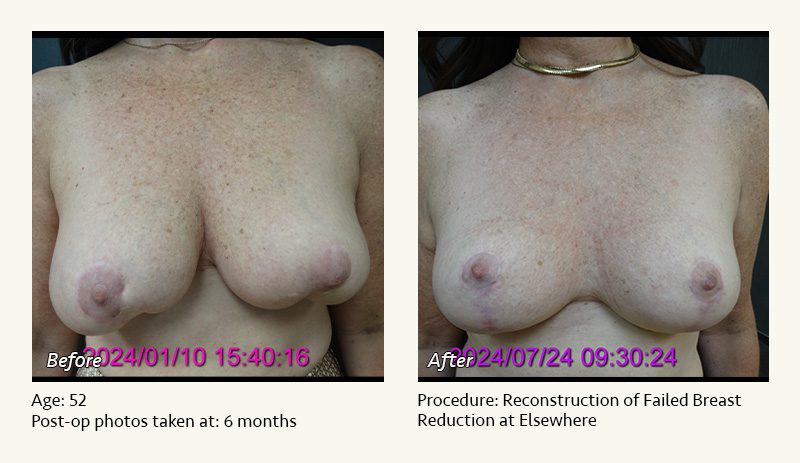
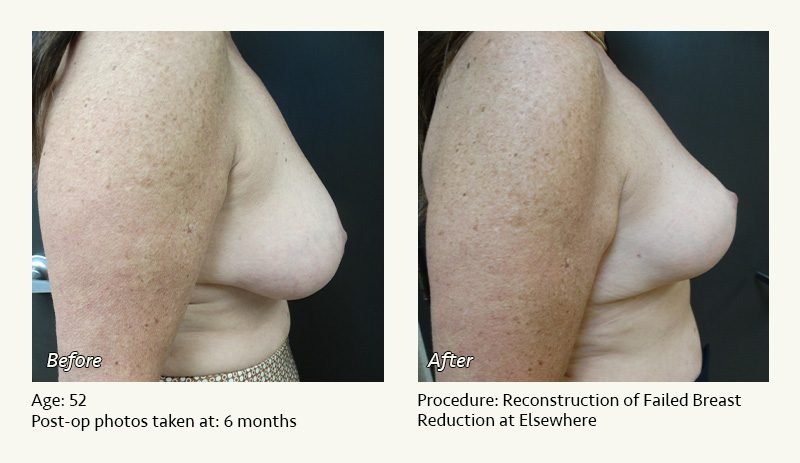
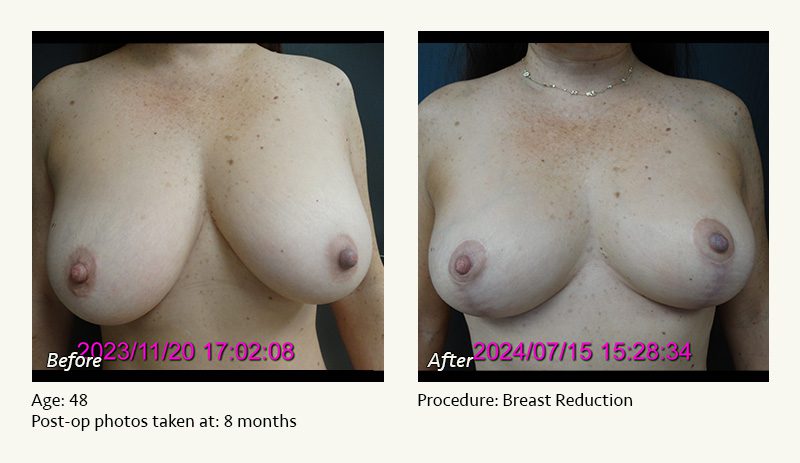
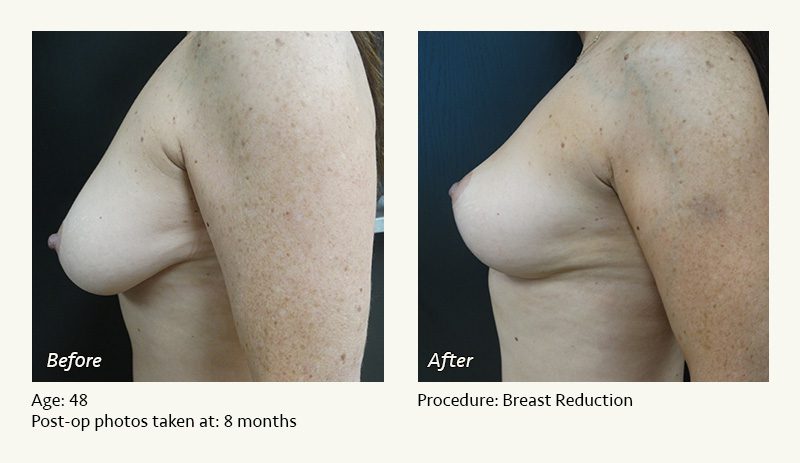
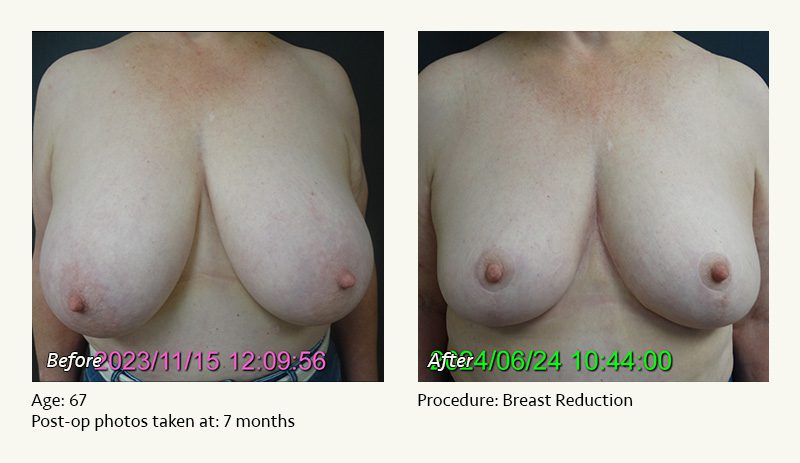
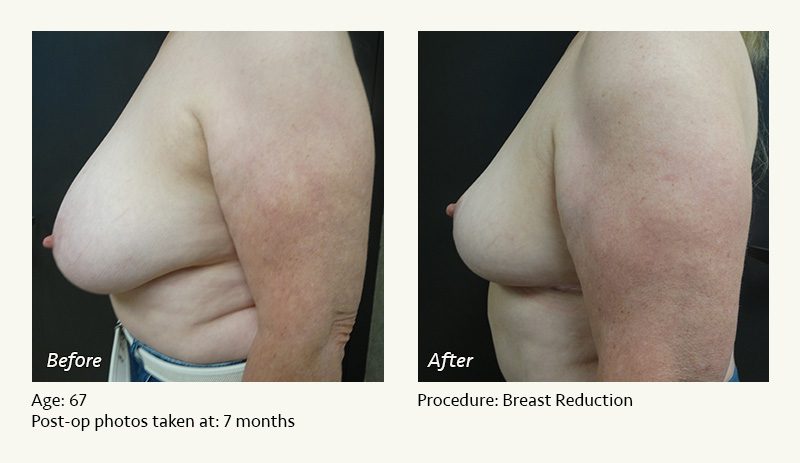
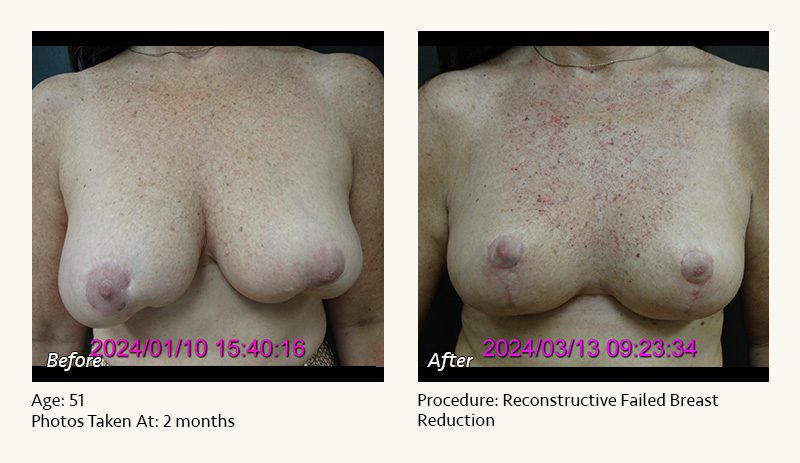
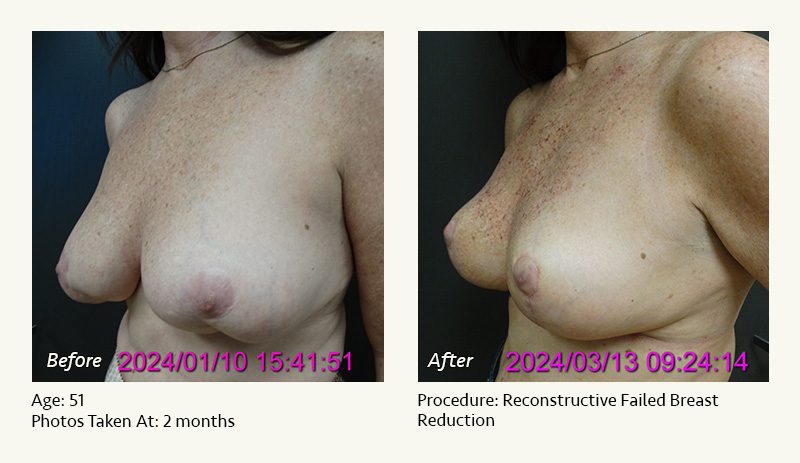
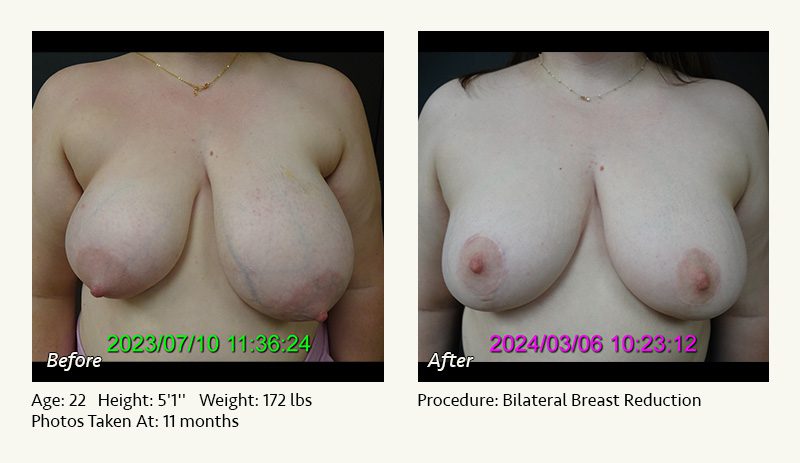
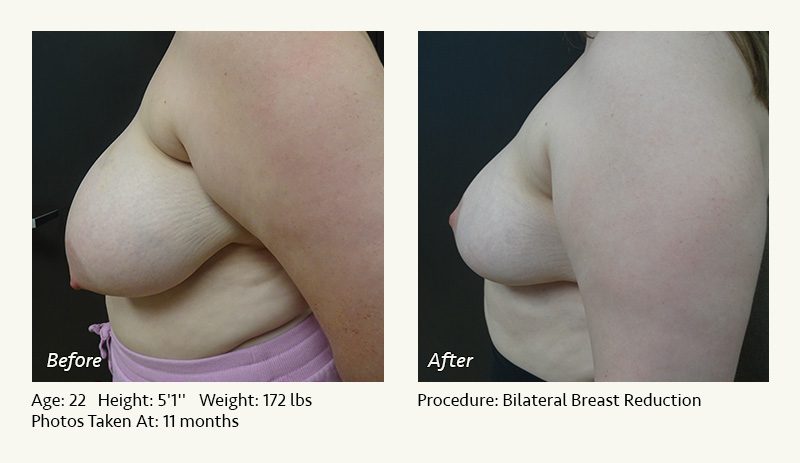
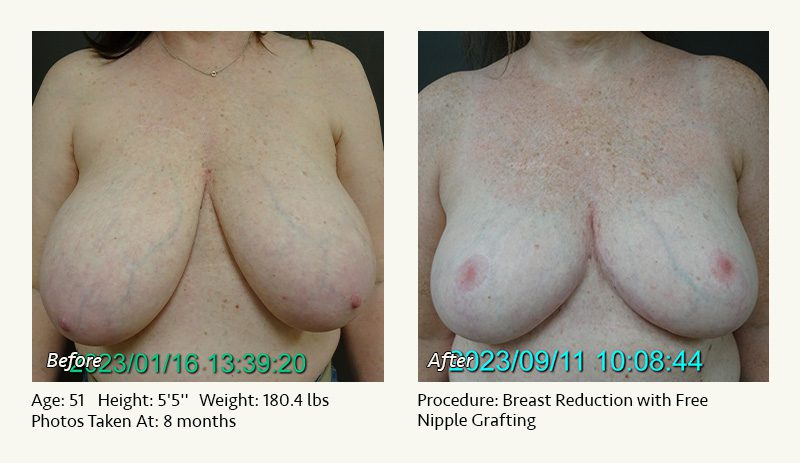
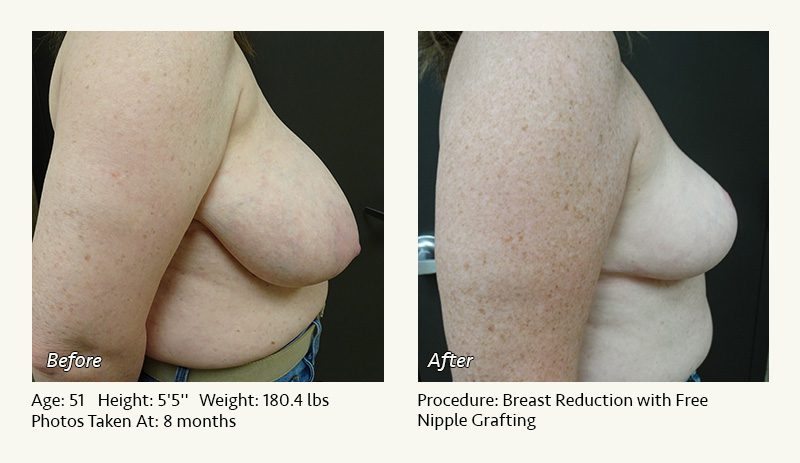
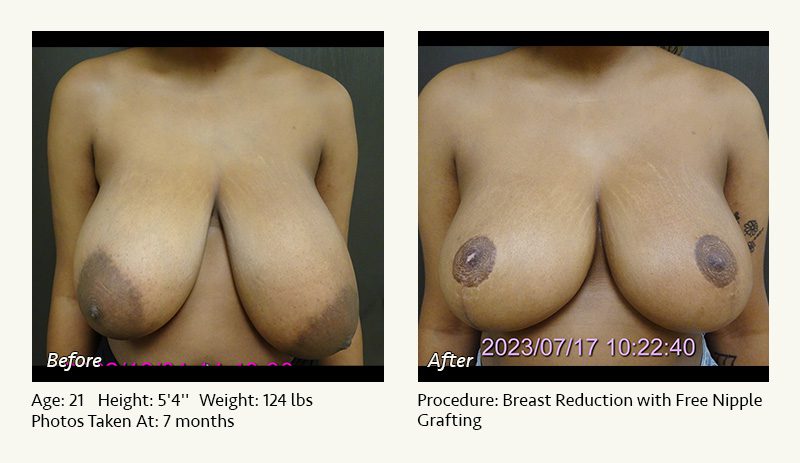
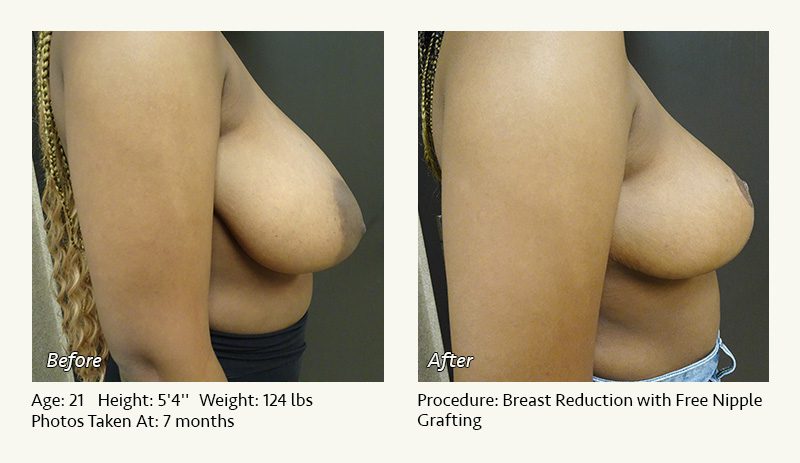
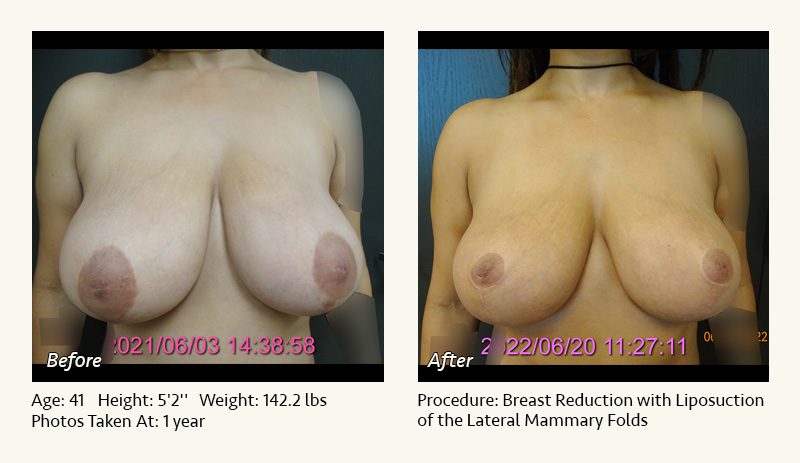
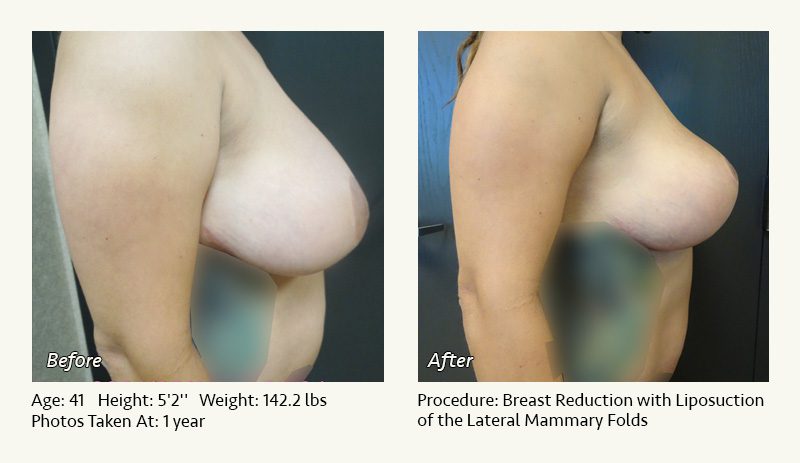
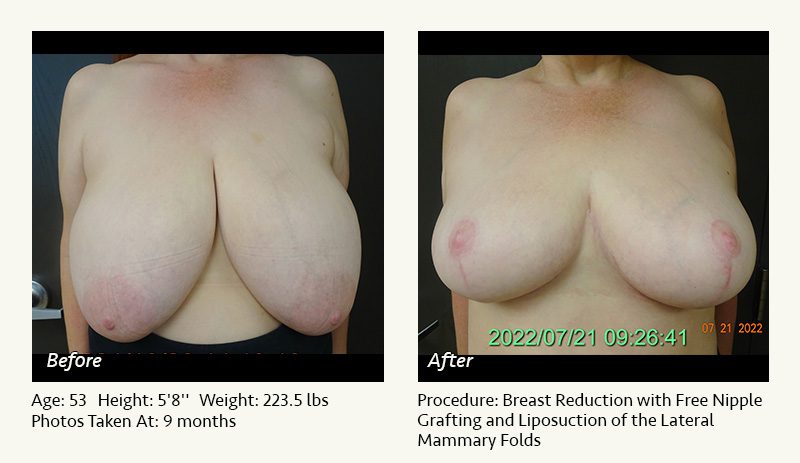
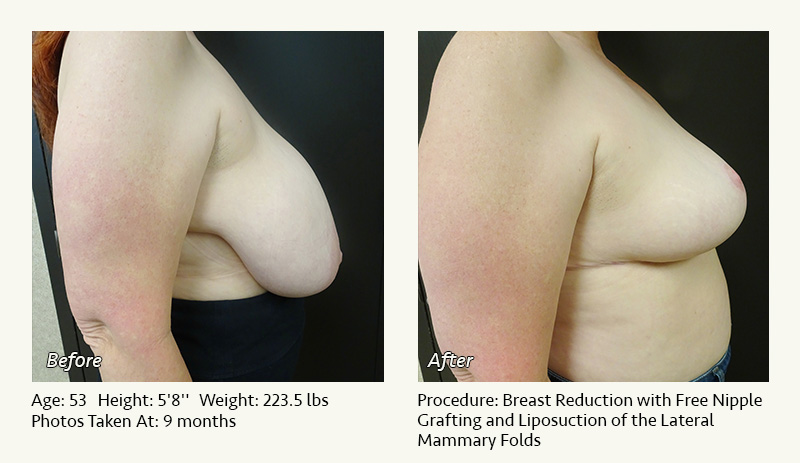
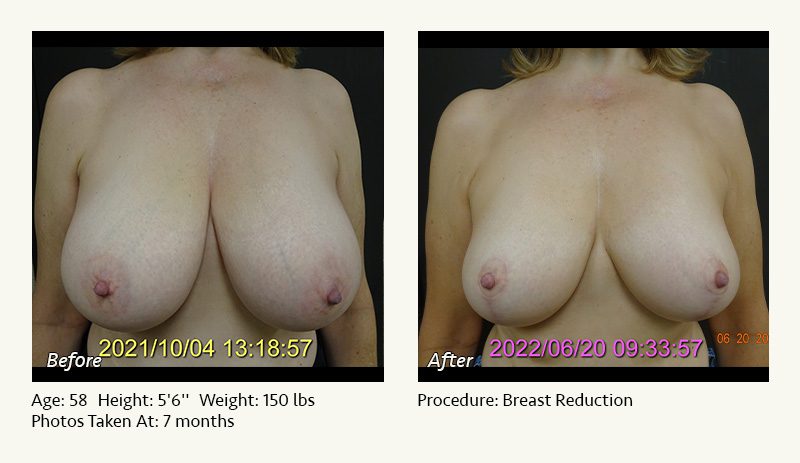
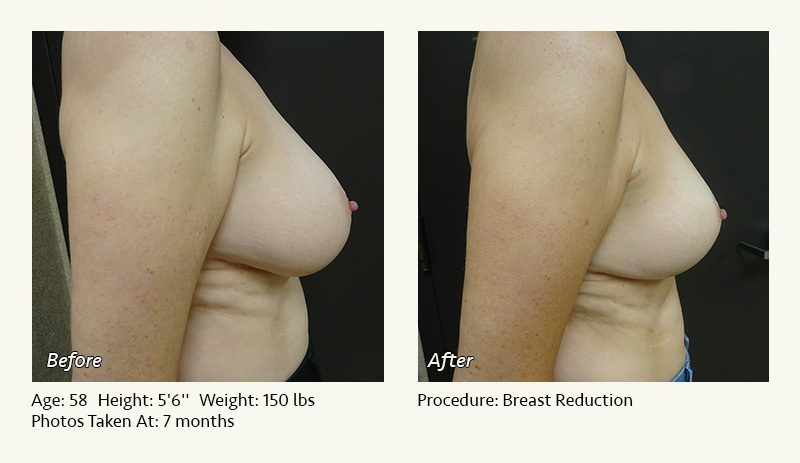
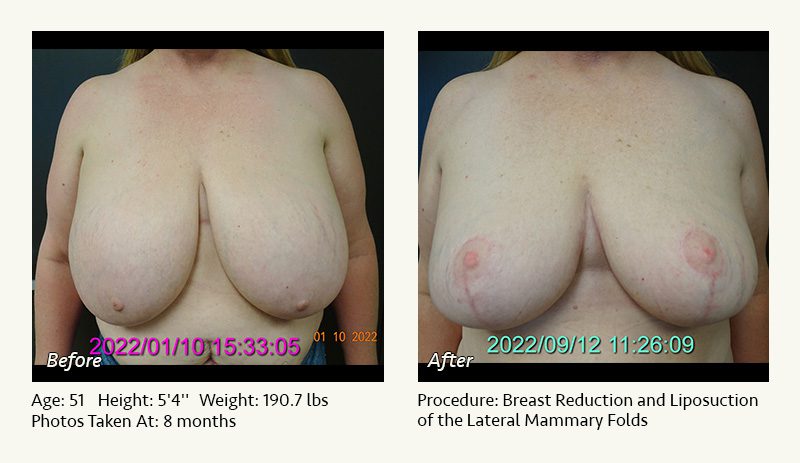
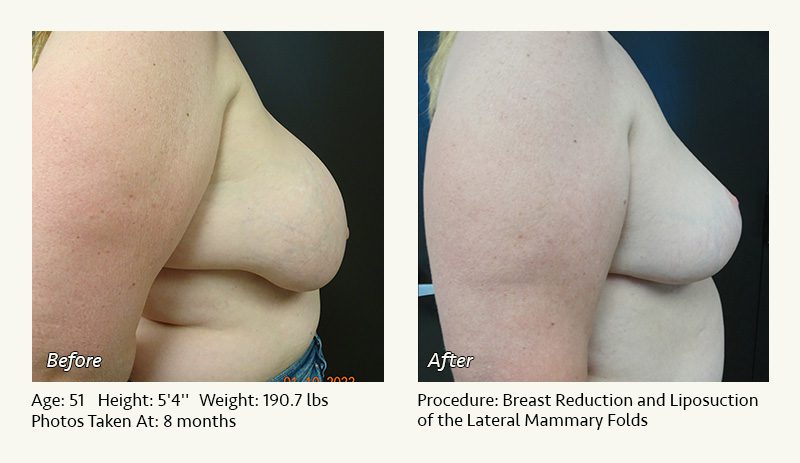
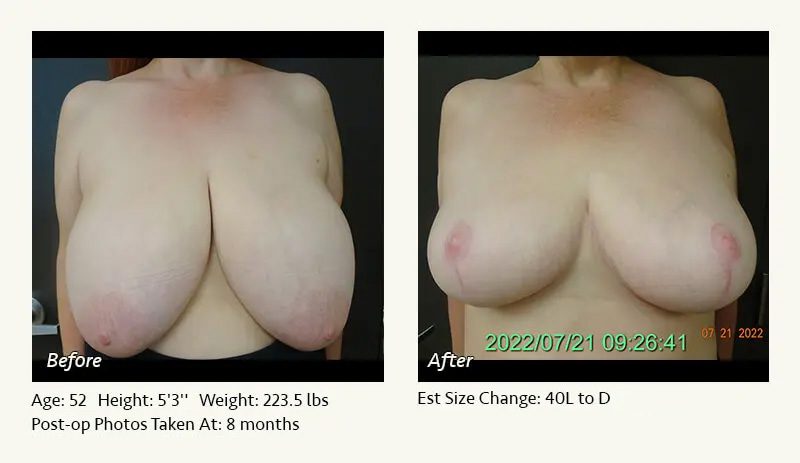
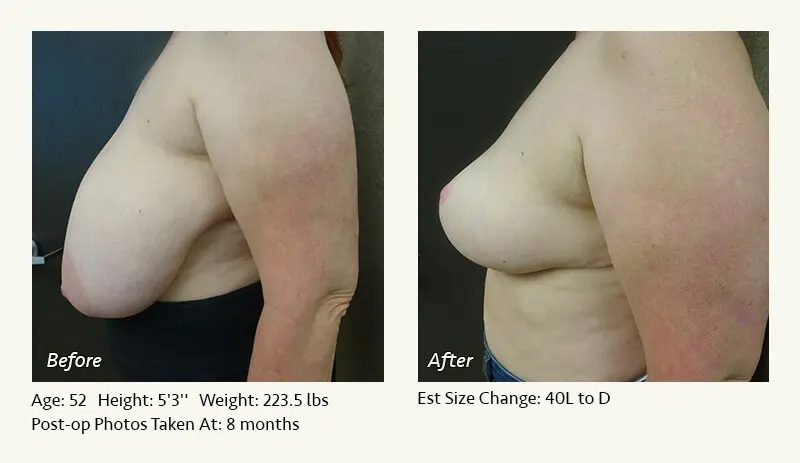
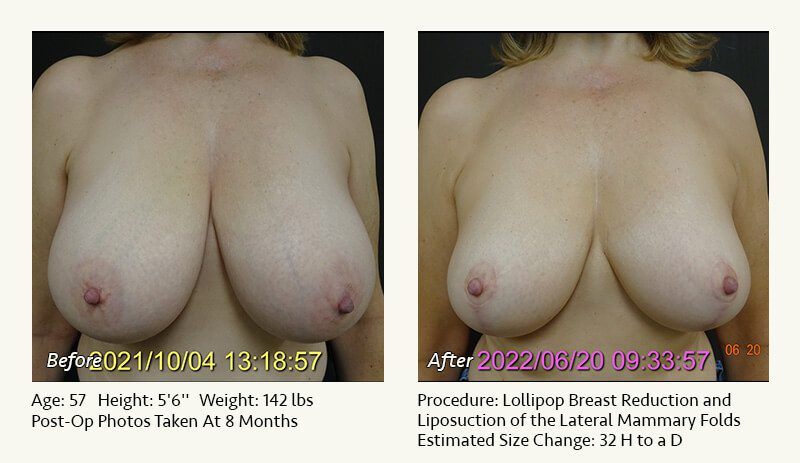
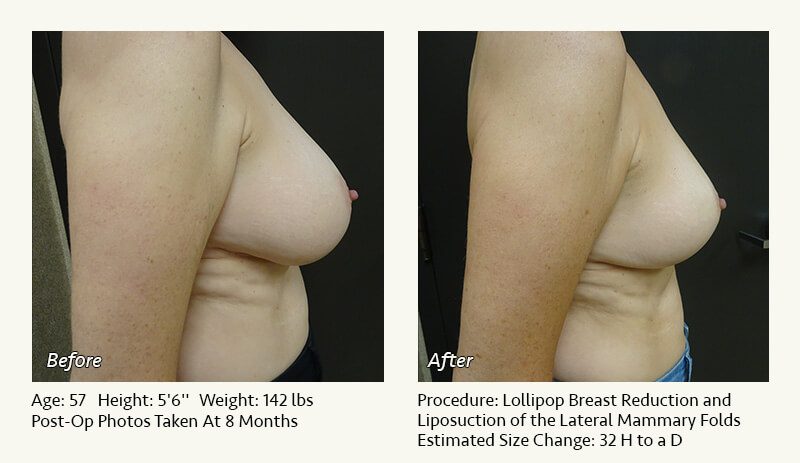
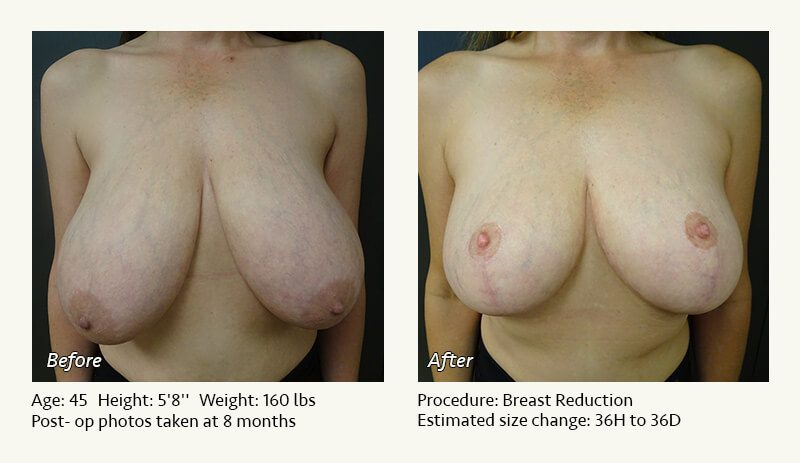
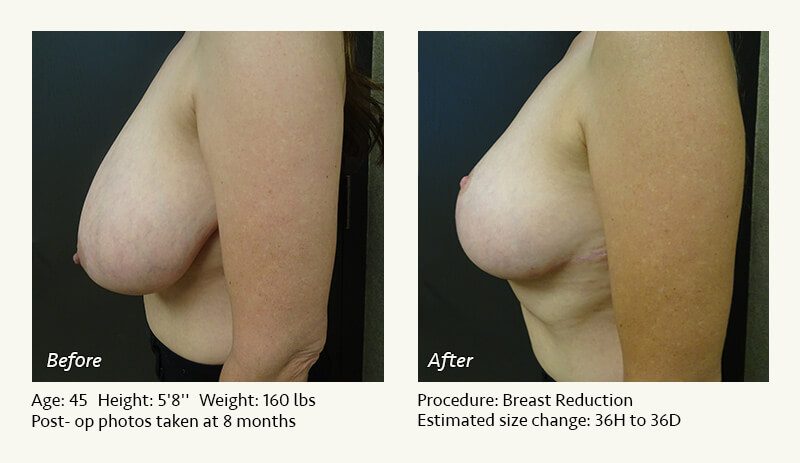
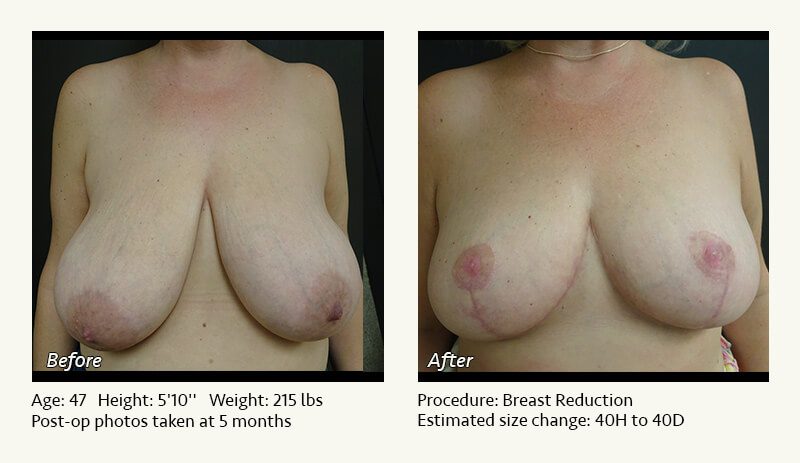
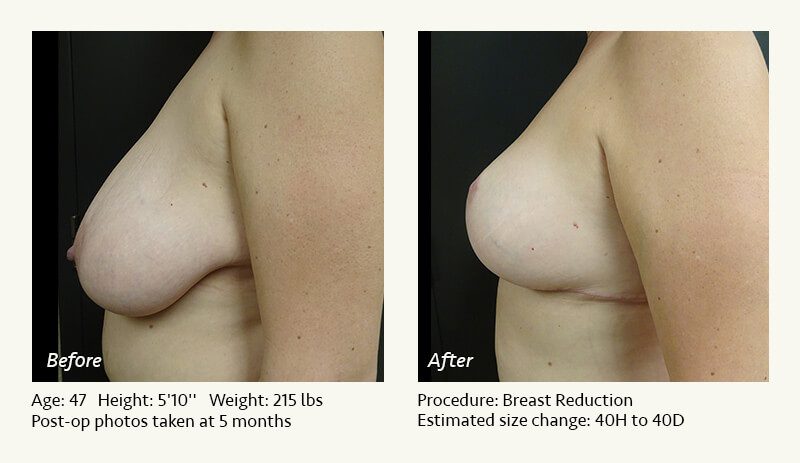
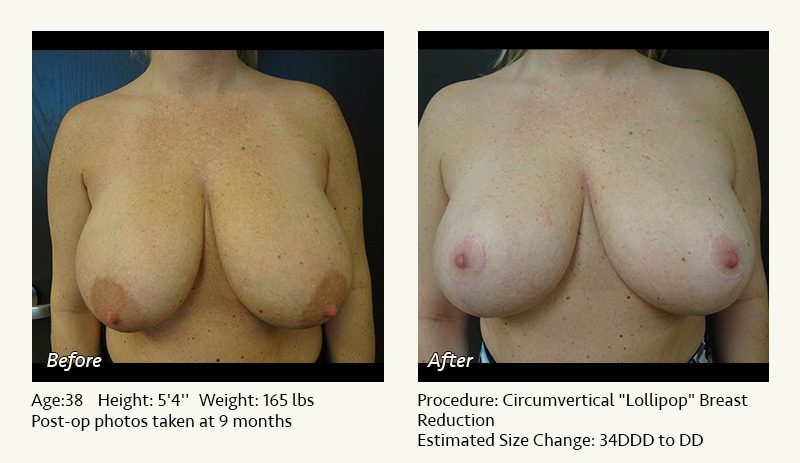
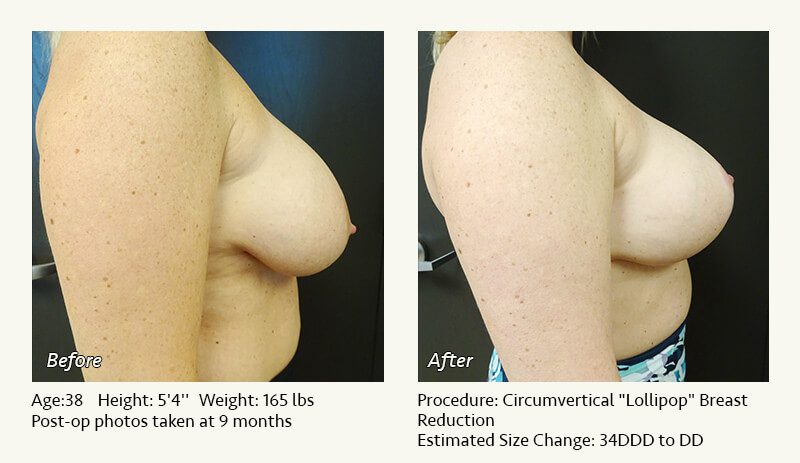
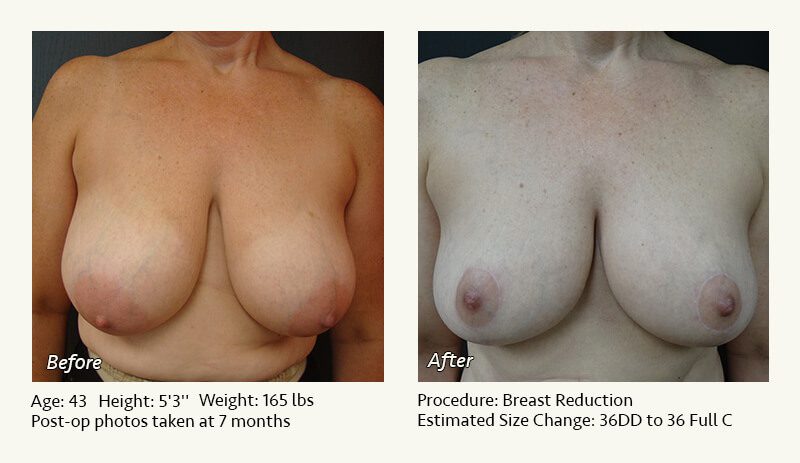
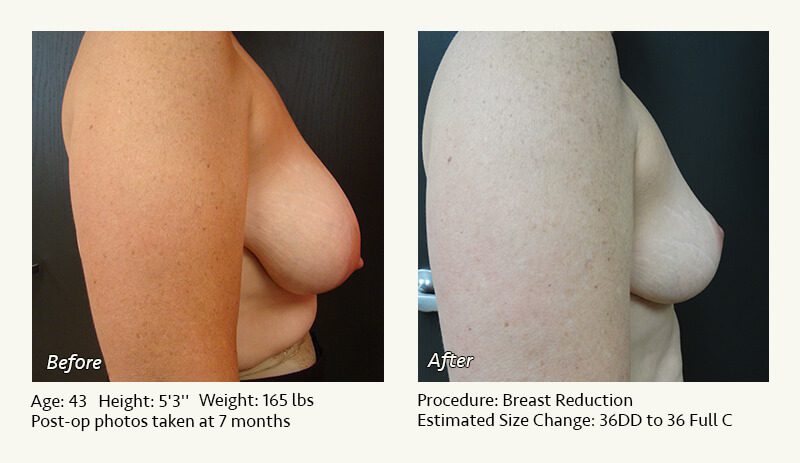
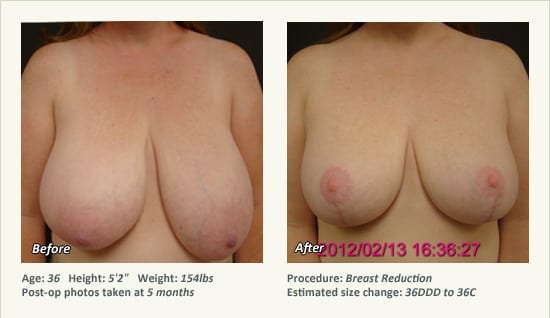
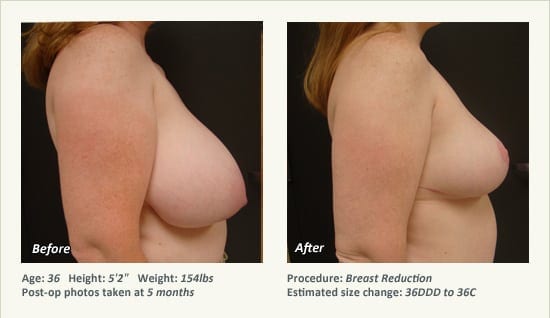
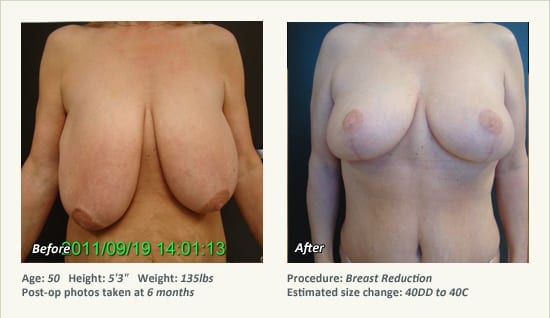
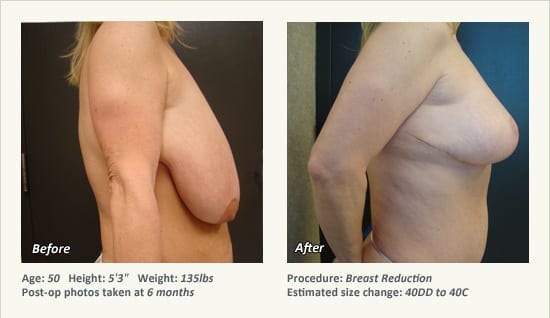
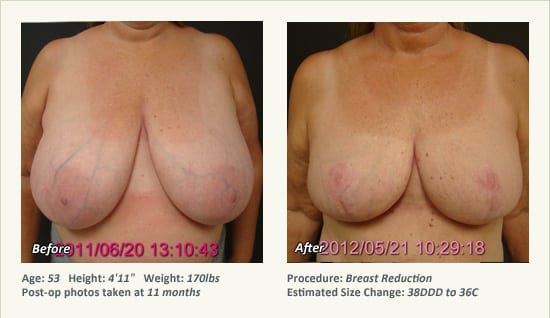
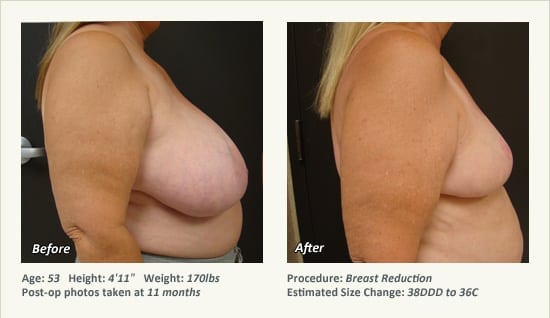
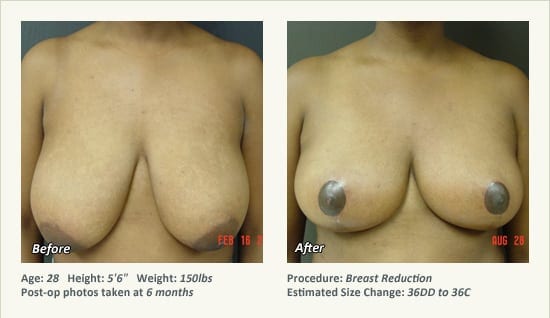
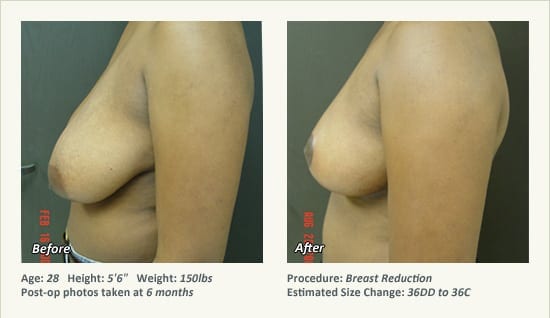
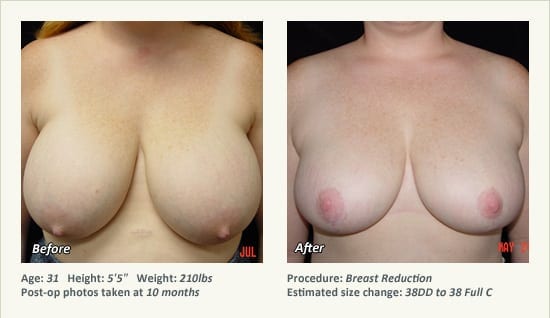
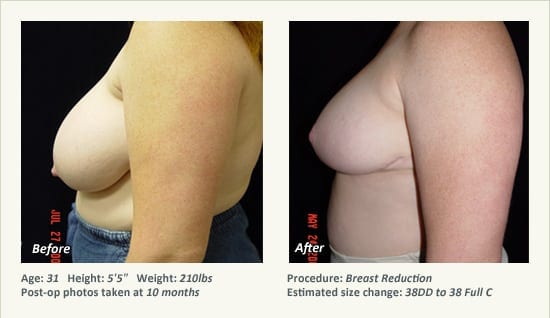
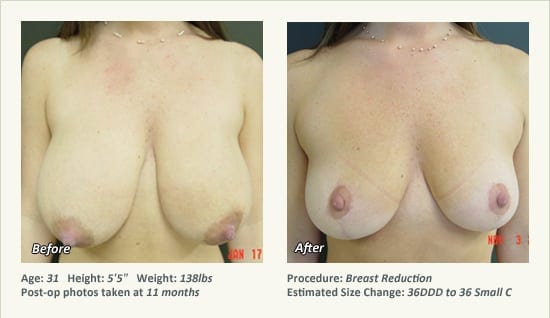
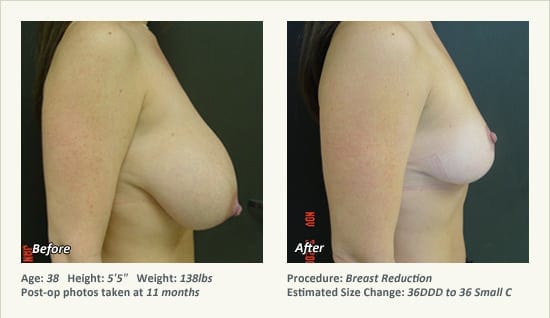
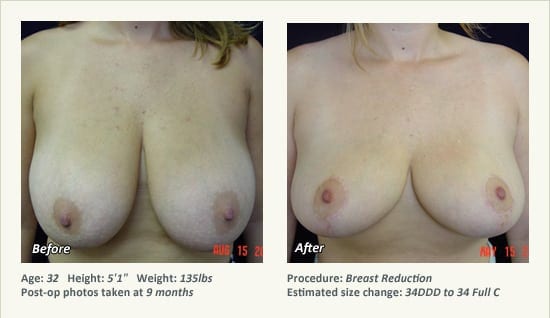
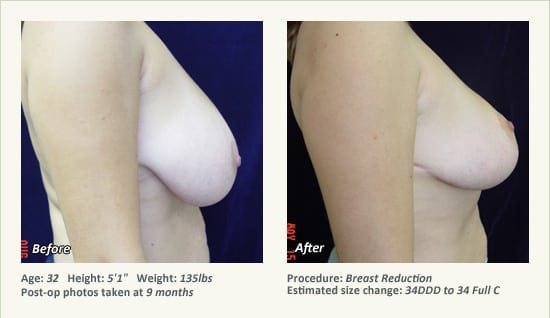
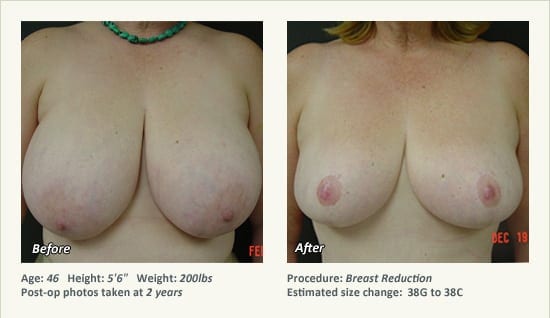
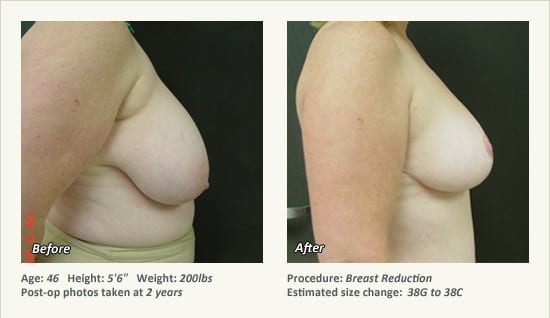
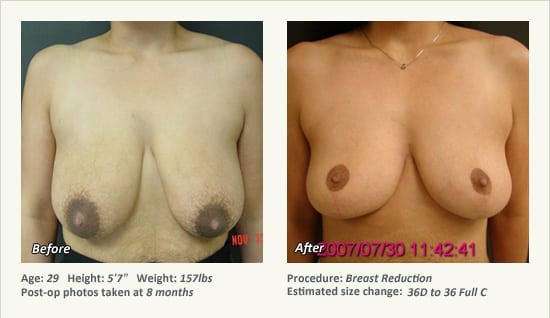
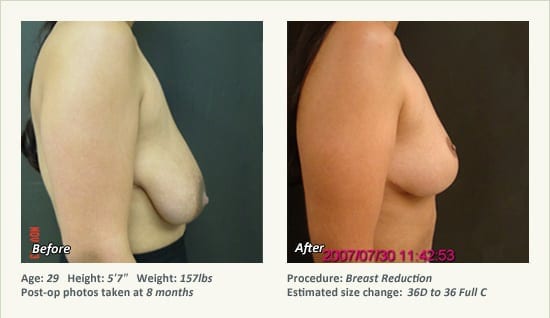
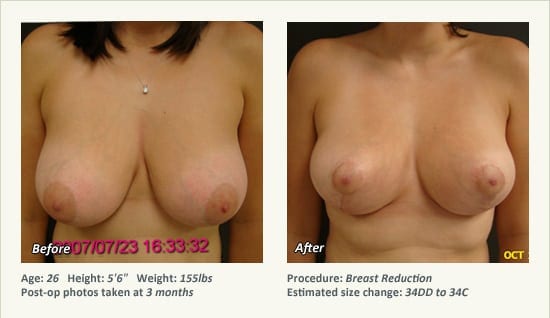
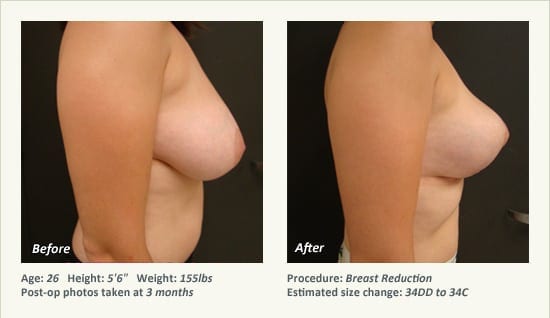
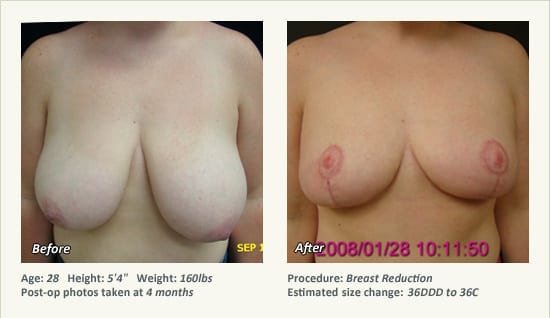
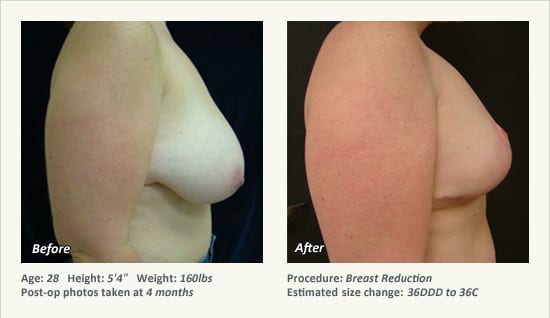
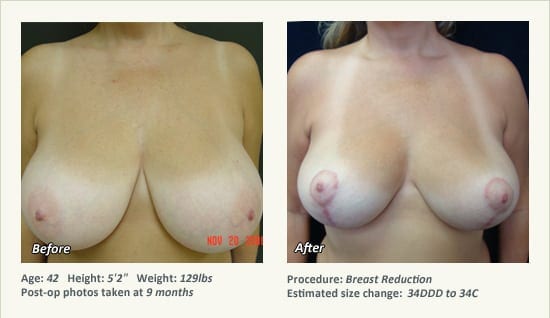
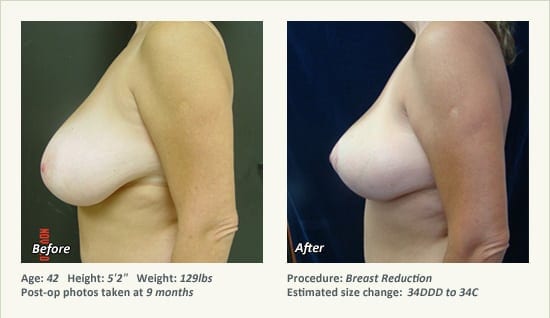
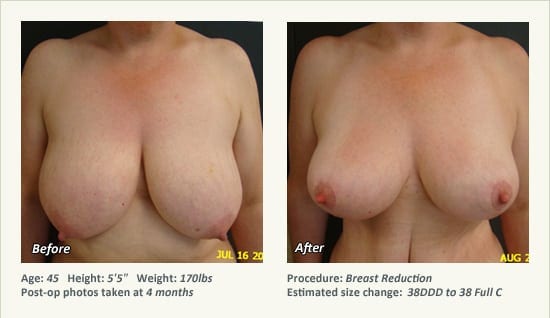
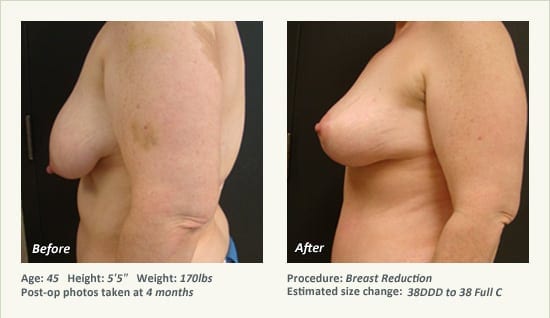
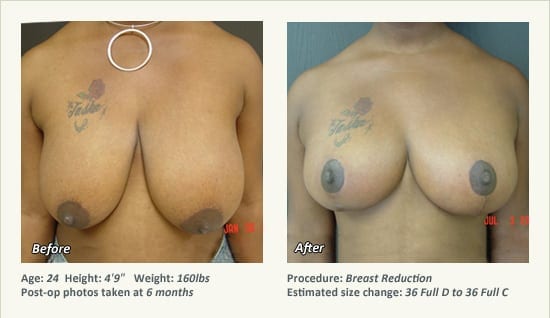
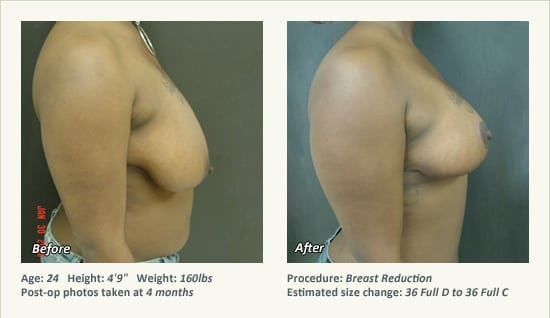
Dr. Friedman in Plano, Texas performs breast reduction under general anesthesia on an outpatient basis. The procedure is performed at Dr. Friedman’s private surgical facility, the West Plano Plastic Surgery Center, located on the campus of Texas Health Presbyterian Hospital of Plano. He exclusively uses physicians—not nurses or technicians—to administer your anesthesia. Incisions are placed around the nipple-areola and the lower portion of the breast. There are no incisions on the upper breast. Most of the stitches are internal, and all are absorbable. Although there are scars from surgery, they fade significantly over time.
Temporary drains are usually necessary and are removed during the first postoperative visit. Pain is generally mild to moderate and well-controlled with prescription pain medication. Most patients return to light activities within 3 to 5 days. Heavy lifting and chest work-outs should be avoided for 6 weeks.
When you visit our office in Plano, Texas, we will be happy to show you what to expect from breast reduction. We will also show you a variety of “before and after” photos of breast reductions performed by Dr. Friedman. If you wish to speak to other women who have undergone the procedure, we will be happy to provide phone numbers.
Q & A: Breast Reduction
-
Will my breasts be lifted during my breast reduction?
All breast reductions involve lifting the breasts. Although the primary reason for surgery is reduction of back and neck pain, the breasts generally look much better after surgery. In addition, the nipple-areolae are reduced in diameter and moved higher on the breasts, so that they point forward (rather than down).
-
What size will my breasts be after reduction?
This is an individual decision. However, Dr. Friedman usually recommends a postoperative size in the C to D range. The idea is to remove enough breast tissue to improve your symptoms and appearance–without removing so much tissue that you feel there’s nothing left.
-
How visible are the scars?
Every woman scars differently. However, the scars around the nipple-areolae and along the upper portion of the vertical incision are generally fine line and relatively inconspicuous. The lower part of the vertical scar and, if utilized, the incision within the crease under the breast frequently widen to some degree, as these portions of the scars bear the most weight and tension. The scars are clearly a trade-off for the improvements anticipated with surgery. For most women, this trade-off is very worthwhile.
-
Should I lose weight before breast reduction surgery?
Many women with enlarged breasts are overweight. Dr. Friedman does not require that you lose weight prior to surgery. However, if you do plan to lose weight, you should do so before surgery, rather than afterwards. If you lose a large amount of weight after surgery, you may experience some recurrent sagging of the breasts.
Breast Reduction: Instructions
One week before surgery
- Do not take aspirin-containing products, as these may increase your risk of bleeding. Use extra-strength Tylenol for any headaches or other minor pains.
- Please notify Dr. Friedman’s staff if you become sick with a fever, significant cough, etc. If necessary, your surgery can be rescheduled to a time when you are feeling better.
- Do not smoke at all or use a nicotine patch for at least two weeks (and preferably 4 weeks) prior to surgery and 4 weeks after surgery. Smoking interferes with wound healing and increases your risk for anesthetic and surgical complications.
- Arrange to have a relative or friend drive you home after surgery and stay with you for the evening. You cannot drive yourself home.
The evening before surgery
- Do not eat or drink anything for at least 8 hours prior to your scheduled surgery time.
- Make some jello and/or soup for after surgery. Have some juice in your refrigerator.
- The anesthesiologist will contact you by phone to discuss your medical history and to answer any questions.
Day of surgery: before you leave home
- Remember not to eat, drink, or smoke. This includes no chewing gum, mints, etc.
- Make sure someone is available to drive you home. Put a pillow and blanket in the car.
- Wear loose, comfortable clothing. Avoid heavy make-up, jewelry, or contact lenses. Please do not use any lotion, baby oil, perfume or powder. LEAVE ALL VALUABLES AT HOME!
Day of surgery: at the facility before surgery
- Dr. Friedman will talk to you before surgery to answer any last-minute questions. He will place drawings on your chest to help him accurately plan your surgery.
- You will meet the anesthesiologist and surgical nurses.
Day of surgery: at the facility after surgery
- You will be taken to the recovery area to wake up after surgery. Dr. Friedman will go to the waiting room to speak to your family/friends.
- Approximately 1 hour later, your family can visit you. Once you are feeling well enough, you may go home.
At home after surgery
- Have someone stay with you for the first night. You may be weak and drowsy.
- Take the antibiotics, pain medication (as needed), and anti-nausea medicine (if needed) that Dr. Friedman has prescribed for you.
- Sleep with your head elevated. Sleep on your back (not your stomach or side).
- Keep your dressings (gauze and tape) clean and dry. Do not remove the dressings. You may shower only from the waist down. You may wish to sponge bathe.
- If you have drains, measure and empty the fluid from the drains twice daily. After emptying the fluid, re- collapse the drains to ensure proper function. Keep a record of drain output and bring it to Dr. Friedman’s office for your first follow-up visit.
- Take at least 10 deep breaths every hour. This will help keep your lungs expanded.
- Do not be a couch potato. To reduce the risk of blood clots in the legs, get up and walk any time you eat or need the bathroom. While you are in bed, repeatedly flex your ankles (moving your toes up and then down) and/or have your family massage your calves.
- If you experience a prolonged fever (oral temperature greater than 101), contact Dr. Friedman. Feel free to call our office or to page Dr. Friedman for any other problems or concerns.
Instructions for your first postoperative visit (about one week after surgery)
- Activity level
1 Week after surgery: you may resume casual walking but must not engage in vigorous exercise that increases your blood pressure or heart rate. You may resume driving once you are off of your pain medication. Avoid freeways until you are comfortable with city driving.
3 Weeks after surgery: you may resume jogging (with a jog bra) or an elliptical trainer but must avoid vigorous use of your chest or arms.
6 Weeks after surgery: you may gradually resume exercise involving the chest and arms. Only now may you lift more than 5 pounds. - Sleeping position
Please sleep on your back (flat or elevated) or part way over (pillow under your shoulder and hip). Do not sleep on your side until about 3 weeks after surgery. Unless otherwise instructed by Dr. Friedman, do not sleep on your stomach until about 8 weeks after surgery. - Incision care
You have a layer of tissue glue to seal your incision. After this peels off (about 2 weeks after surgery), begin scar massage with Prosil twice daily. Prosil, a liquid silicone gel, is available at our front desk. We also recommend silicone gel sheeting, which you can purchase over the internet. Continue scar massage for about 3 months. You should also massage the outer torso adjacent to the breasts (if liposuction was performed in this area) 15 minutes daily for about a month. - Bra usage
You may begin use of a bra, ideally a sports bra or one that fastens in the front. Do not wear an underwire bra for at least 3 months following surgery unless instructed to do so by Dr. Friedman. - Water exposure
You may begin light showers 48 hours after your drains are removed. You should avoid scrubbing your incisions. Do not immerse your breasts under water in a bathtub for 4 weeks. Avoid immersing your breasts in a pool, lake, or ocean for 6 weeks. - Medications
One week after surgery, you may resume use of any medications or supplements that you discontinued prior to surgery. However, for at least 3 weeks, you should avoid Motrin, aspirin, and any other product that may thin your blood. - Smoking
Do not smoke for at least one month (and preferably much longer) after surgery. Smoking may increase your risk of infection, lung problems following anesthesia, and wound healing problems. - Tanning
You may tan your breasts whenever you like. However, you should avoid tanning directly over your incisions for at least 6 months. Premature tanning of the incisions may cause them to darken permanently. - Sex
You may resume intercourse in a non-weight bearing position (i.e. on your side) about 3 weeks after surgery. You may not bear weight on your chest for at least 6 weeks. - Breast shape
Your breasts may look too high and too “square” right after surgery. They will gradually settle and become more round over the next several months.
Please feel free to ask Dr. Friedman or his staff about any additional questions or concerns.